I recently saw NHS data on unplanned or emergency hospital admissions for people with multiple sclerosis in our five hospitals that constitute Bart Health NHS Trust. At the top of the list were gastrointestinal problems, with faecal impaction being the most likely culprit. This is tragic as faecal impaction is preventable and potentially has knock-on consequences for people with MS.
Many people with multiple sclerosis (MS) seem content to live with chronic constipation, i.e. it becomes part of their new normal. Ideally, pwMS should have a bowel action daily or at least 3-4x times per week; anything less than this may put you at risk of complications from poor gut hygiene or poor gut health.
I have written about intermittent diarrhoea in MS being a sign of possible faecal impaction and how to manage it (see Intermittent diarrhoea in MS; 02-Nov-2021) and the issue of faecal incontinence (see Faecal incontinence; 4-Aug-2021). Another issue associated with chronic constipation in MS is small intestinal bacterial overgrowth (SIBO).
Small intestinal bacterial overgrowth (SIBO)
SIBO is defined as an increase in the bacterial content of the small intestine above normal values. It is common in pwMS. In the study below from China, close to 4 in 10 pwMS had SIBO. SIBO is detected in approximately a third of patients with gastroenterological complaints who undergo a breath test. SIBO is associated with smoking, bloating, abdominal pain, and anaemia. Proton pump inhibitors (omeprazole and related drugs) are a risk factor for developing SIBO. The risk of SIBO increases with age and does not depend on gender or race.
SIBO is associated with dyspepsia, irritable bowel syndrome, abdominal bloating, functional constipation, diarrhoea and faecal impaction. SIBO is associated with a slowdown in your bowel transit time, which decreases the normal clearance of bacteria from the small intestine. The slowdown of this transit is due to changes in the motility of the intestine that is almost universal in pwMS.
Diagnosis
The commonest test that is done to diagnose SIBO is a breath test. It is a noninvasive test that measures the amount of hydrogen or methane you breathe out after drinking a mixture of glucose and water. A rapid rise in exhaled hydrogen or methane indicates bacterial overgrowth in your small intestine. Although widely available, breath testing is less specific than other tests for diagnosing bacterial overgrowth.
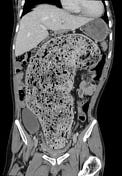
The gold standard for diagnosing SIBO is a small intestine aspirate and fluid culture. The fluid sample is obtained as part of a small bowel endoscopy. Other ancillary tests included can include abdominal X-rays or CT scans. I often diagnose faecal impaction when I look at spinal MRI scans. MRI evidence of constipation is widespread in pwMS.
Treatment
The initial way to treat bacterial overgrowth is to manage the underlying bowel hypomobility problem and to clear any faecal impaction that may be present. In parallel, you may require a course of antibiotics. A course of antibiotics reduces the number of abnormal bacteria in the bowel. However, unless you deal with the underlying problems, the bacteria will repopulate the bowel when the antibiotics are discontinued. This is why some people with SIBO may require long-term antibiotics. Switching between different antibiotics helps prevent bacterial antibiotic resistance from emerging. Please be aware that antibiotics wipe out most intestinal bacteria, both normal and abnormal and hence are not an ideal long-term solution to SIBO.
An important part of treating SIBO is for you also to start a gut health programme. You will need a nutritional review and may need to change your diet to prevent constipation and/or faecal impaction. Seeing a dietician may help; depending on your diet, you may need supplements. The latter is particularly relevant if you are vegan (Please see my blog post ‘Calling all Vegans’; 6-Mar-2019).
SIBO may damage the bowel, i.e. bacteria can produce toxins that can directly damage the intestinal surface or mucosa. This can result in leaky gut syndrome and acquired lactose intolerance. The leaky gut syndrome is controversial and associated with many symptoms that may overlap with MS-related symptoms. Leaky gut syndrome is not a medically defined condition, and no specific tests or treatments are available. In comparison, acquired lactose intolerance is when someone loses the ability to digest lactose, the main sugar in milk, which causes you to develop diarrhoea, gas and bloating after eating or drinking dairy products. If you have lactose intolerance, you quickly learn to avoid lactose-containing products or use lactase preparations that help digest lactose. Please note cheeses and yoghurt are generally tolerated because the bacteria used in the culturing process to produce these dairy products break down the lactose.
Bacterial overgrowth
We know that many bacterial overgrowth products can impact human metabolism and behaviour. People with liver dysfunction can’t metabolise these bacterial toxins and develop hepatic encephalopathy. People with neurological disorders with reduced brain and cognitive reserve tend to be more susceptible to the effects of these bacterial metabolites, which are thought to upregulate innate immunity in the nervous system. This is why I try and stress to my patients that they should manage their constipation to prevent this from happening. Severe constipation and faecal impaction should be viewed as a chronic infection and managed and treated as such.
I would like to know how many of you are aware of SIBO, if any of you have been investigated for SIBO and if any of you are on treatment to reduce bacterial overgrowth. If you have time, please complete a short online survey. In parallel, please feel free to share your experiences of SIBO and the effect that treating SIBO has had on your symptoms of MS.
Research Paper
Objective: It's hypothesized that gastrointestinal microbiota might play an important role in pathogenesis of multiple sclerosis (MS). The aim of the present study was to assess the prevalence of small intestinal bacterial overgrowth (SIBO) in MS patients compared with sex and age matched controls without MS.
Methods: The present study was a case-control type, it included 118 patients with definitive MS and 118 age-sex matched controls. Progression of disability was assessed using the Multiple Sclerosis Severity Score (MSSS). All patients and controls underwent the glucose breath test to assess SIBO.
Results: Forty-five of the 118 MS patients were SIBO positive (38.14%; 95%CI: 29.37%-46.90%) compared with 10 of 118 in the control group (8.47%; 95% confidence interval [CI]: 3.45%-13.50%); the difference was statistically significant (P<0.0001; Odds ratios (OR), 4.50; 95% CI, 2.38-8.50). In addition, 102 out of the 118 patients (86.4%) presented at least one GI symptom. Constipation (78.0%), Bloating (46.6%), and fecal incontinence (44.1%) were common. Multivariate analysis showed that expanded disability status scale (EDSS) score and MSSS were the only factors associated with the SIBO-positive status in MS patients (OR, 3.44; 95% CI, 1.56-6.99; and OR, 2.76; 95% CI, 1.42-4.94, respectively).
Conclusion: SIBO is highly prevalent in Chinese patients with MS. Further analytical work is required to establish a causal association between SIBO and MS risk and progression.
Subscriptions and donations
Paid subscriptions to MS-Selfie are being used to administer the Newsletter and associated MS-Selfie microsite, which is now open to all readers. At the request of several readers, I have now added the option of making a one-off donation. To keep this initiative open to all readers, I would appreciate it if those who can afford a subscription to subscribe. For active paying subscribers, thank you; your contribution is much appreciated. Because of the falloff in paying subscribers, I am considering returning to a paywall that will give paying subscribers six months of unlimited access to all newsletters. At the same time, free subscribers will have a wait to access the newsletters later, not as an email, but on the substack site.
General Disclaimer: Please note that the opinions expressed here are those of Professor Giovannoni and do not necessarily reflect the positions of Barts and The London School of Medicine and Dentistry nor Barts Health NHS Trust. The advice is intended as general and should not be interpreted as personal clinical advice. If you have problems, please tell your own healthcare professional, who will be able to help you.














Share this post