As you are aware people with MS are much more likely to split with their partners and to be living alone. Social isolation and loneliness are common problems for people living with MS. So if you are living alone please read this newsletter.
Case study
One of my patients on ocrelizumab who is triple vaccinated contacted me on Monday to tell me she has COVID-19. Fortunately, she is not doing too badly and is at home. During the early part of the pandemic, she read my blog post on self-monitoring and bought herself a pulse oximeter. At the moment her saturations are above 92%. I have told her she needs to make sure she has antigen-positive and/or PCR-positive COVID-19 and tries to get a formal NHS antibody test done to see if she has seroconverted after her three vaccines. This is to prepare herself for being eligible for Ronapreve if her condition worsens.
The current NHS guidelines for Ronapreve (casirivimab and imdevima) are:
Hospitalised specifically for the management of acute symptoms of COVID-19
SARS-CoV-2 infection is confirmed
Negative for baseline serum anti-spike antibodies against SARS-CoV-2
The other good news is that my other ocrelizumab-treated, double-vaccinated, antibody-negative patient who has been admitted with worsening COVID-19 was treated with Ronapreve on day 5 of her admission and was discharged home yesterday off oxygen. This is very reassuring in that the NHS has gotten its act together and there are now treatment options for COVID-19 that is saving lives. This is also telling us that we are now learning to live with COVID-19.
Pulse oximetry
Early on during the COVID-19 pandemic a young surgical trainee tragically died alone at home from COVID-19 in Belfast. He probably died from pulmonary complications of COVID-19 that had gradually crept up on him and by the time he needed hospitalisation and ventilatory support he was probably too unwell to do anything about it. A big issue is that as you become hypoxic (lack of oxygen) your thought processes become clouded and your ability to make a judgement about your own health become erratic.
I know of two close colleagues who self-isolated with COVID-19 and both of them developed severe exertional shortness of breath at the height of their infection. My one colleague said he could barely make it from his bed to the toilet due to shortness of breath. Fortunately, both have made a recovery now and are doing well.
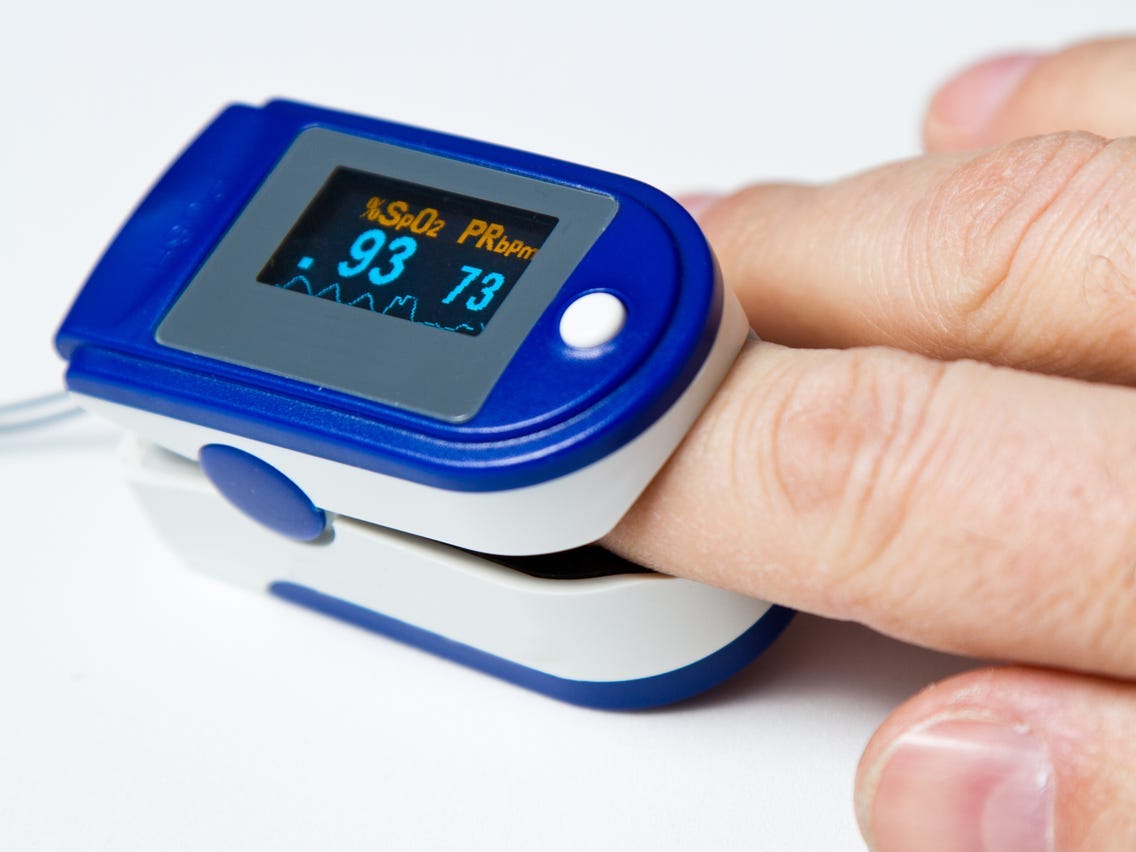
A third colleague who recovered from COVID-19 was bed-bound for two weeks and was on the verge of calling an ambulance, but decided against it. Fortunately, his wife is a GP and was monitoring him at home with a pulse oximeter, a device to measure how much oxygen is in your blood, that she uses for home visits. This colleague told me that he did try and call 111 and after waiting 90 minutes hung up. Waiting ninety minutes or longer for advice and to then be told to call an ambulance could be the difference between life and death.
When I was redeployed in the first wave of the pandemic we didn’t have to physically examine the chests of patients admitted with COVID-19, we mainly assessed how well their lungs are functioning based on their oxygen saturation in their blood relative to how much oxygen they are getting, be it from room air (21% oxygen) or via a nasal cannula or face mask. When we use a nasal cannula or a face mark we deliver oxygen at different flow rates and this is also taken into account.
In general, most people have an oxygen saturation rate above 94%. It does vary with age and altitude. It is relatively easy to measure yourself, but you need to have a pulse oximeter. In early COVID-19 pneumonia, exertional oxygen saturation levels fall first, i.e. if you attempt to walk or exercise and your blood saturation levels fall, for example, below 90% despite being normal at rest. This would indicate that your lungs are in trouble and that you probably need to go to the hospital. People with COVID-19 can deteriorate very rapidly, i.e. within hours, so having an early warning system should help.
I wonder if the young surgeon above had been monitoring himself with a pulse oximeter and had noticed that his exertional blood oxygen saturation levels dropped with exertion (walking in his home) he would have gotten himself to hospital and survived?
Please note the following symptoms and signs to help identify who has more severe COVID-19 and may need admission to hospital:
severe shortness of breath at rest or difficulty breathing
coughing up blood
blue lips or face
feeling cold and clammy with pale or mottled skin
collapse or fainting (syncope)
new confusion
becoming difficult to rouse
little or no urine output
Oxygen saturation below 90%
Can you imagine trying to pick these symptoms and signs up if you live alone and are self-isolated? I am sure self-monitoring of your peripheral blood oxygen saturation levels, in particular documenting their deterioration, will continue to save lives during the tail of the COVID-19 pandemic.
I purchased my own pulse oximeter online. It is an insurance policy for my family and any of my neighbours or friends who may get COVID-19 and have to self-isolate and self-monitor. Many GP practices can arrange for you to use a pulse oximeter if you are self-isolating and given guidance on how to use them and at what point to call 999.
Please don’t forget the other basics such as prehabilitation and getting vaccinated or having your third or booster vaccine dose.
Subscriptions
All newsletters, such as this one, are free. If you subscribe you will get access to all of the MS-Selfie Case Studies. The MS-Selfie case study from the 12th of November is about managing an immunosuppressed patient who has failed to make an antibody response to the COVID-19 vaccines. In the case study, I discuss the use of Ronapreve and other antiviral agents as potential prophylactic or therapeutic options to prevent or treat COVID-19 in immunosuppressed patients. Please note, subscriptions are being used to employ someone to curate the contents of this and other Newsletters onto an MS-Selfie microsite that I hope will become a living self-help guide for pwMS. If you have MS and can’t afford the subscription please drop me an email and I will arrange a complimentary subscription.
General Disclaimer: Please note that the opinions expressed here are those of Professor Giovannoni and do not necessarily reflect the positions of Barts and The London School of Medicine and Dentistry nor Barts Health NHS Trust. The advice is intended as general advice and should not be interpreted as being personal clinical advice. If you have problems please tell your own healthcare professional who will be able to help you.













Share this post